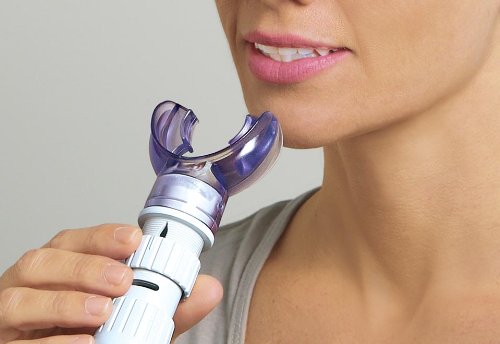
Breathing Trainers & Monitors
Product categories
- Diagnostic Evaluation
- Home & Health & Beauty
- Physical Therapy & Supplies
- Yoga & Sports
POPULAR ITEMS
The breathing simulator is used for chronic bronchitis, bronchial asthma, pulmonary episema, focal pulmonary tuberculosis, angina pectoris, osteochondrosis, stage 1 and 2 hypertension, diseases of the musculoskeletal system.
The particular design of the breathing simulator is based on the adaptation of a breathing catheter model to the specific settings and requirements of the therapeutic uses.
The major limitation of the inhaling simulator is the working time.
It can be used only to maintain the respiratory rhythm for 1-2 minutes for each session.
The future market of the breathing simulator is expected to be in clinical and dental applications.
The presence of the lung expansion capacity and sinus re-epithelialization on X-ray photographs of the lungs.
This has made the diagnosis of disease conditions in the lung easier.
This condition should not be confused with a thickened lung that lacks lung expansion capacity (apparent intra-abdominal fat).
It is a common and easily diagnoseable sign, present in many lung diseases.
The use of breathing simulator in disease therapy should not be confused with simple nebulizer.
With the use of the breathing simulator for the therapy, several benefits can be achieved:
This is due to the formation of normal network and contraction of the bronchial smooth muscle, which is increased and expanded due to the use of an inhaled bronchodilator
During and after the treatment, it is important that proper after care is applied.
Therefore, it is necessary to use a supportive respiratory device.
For an inhaler (bronchodilator), this means using the specialized prosthesis of the lung emphysema patient.
The main function of the respiratory device is the continuous supply of oxygen to the patient, which is divided between two channels, known as a line and a space.
As well as delivery of oxygen the device controls the impedance of the pulmonary blood vessels to the oxygen delivery.
The device is attached to the pharynx via two ports, one of which is exposed to the outside air.
It is controlled by a computer, which controls the dose of the needed inhalant and modifies the dosage based on the amount of oxygen delivered.
The first lung expansion model was developed by Dr. Iosif Popescu and others from the department of medical physics at the Târgu Mureş University of Medicine and Pharmacy, Romania.
The technology was further improved upon by Dr. P. Popescu, Dr. V. Popescu and others in 1996 at the University of Nottingham, UK and in 2007 at the Michigan State University, USA.
Cases of pediatric pneumonia and congestive heart failure were used for testing of this device.
According to Dr. Popescu’s patent No. 7,990,141, Lung Expansion Model “per se” is used.
The model was improved upon by Niederle, P-K and others from the department of physiology and biophysics, German Center for Cancer Research, Germany.
This model was further improved upon by Henniges and other from the department of mechanical engineering, Northern Illinois University, USA.
Practicing doctors and nurses are normally aware of the disease state of the patient and the state of their health prior to administering any form of therapy.